Taking the Fear Factor out of…..Cystocele
This week we are talking about a common diagnosis among women called a cystocele, sometimes also called a prolapsed bladder. The first thing we want to do is to break down the origin of the word. It comes from both French and Greek origins: cysto- meaning “bladder/pouch” and -cele meaning tumor. So essentially, a cystocele is the result of a bladder that has dropped from its original position in the body (anterior to, or “in front of,” the uterus) down toward the pelvic floor and is putting pressure on the vaginal wall. To fully understand what this means, a diagram is very helpful ~ please note that this is a cross section of the body.
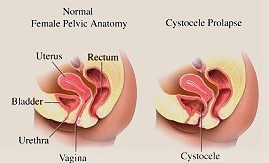
Now that we have a clear picture of what is physically happening in the body when a cystocele is present, let’s talk a bit about what symptoms might be experienced and the available treatments. But first, we want to make one thing very clear: Having a cystocele does not mean that your bladder is falling out of your body!! This is very important to understand, as debunking this myth can eliminate the fear surrounding this diagnosis for a lot of women. Yes, your bladder has descended and may, in some cases, even be felt or seen protruding into the vaginal wall. However, the wall of the vagina serves as a barrier between the bladder and the outside of your body, so it cannot actually come out of your body. Phew!
With the understanding of what a cystocele is (and is not!), we can talk about the common symptoms of a bladder prolapse. The following list of potential symptoms can vary depending on the severity of the prolapse among other factors:
- Slow stream of urine
- Feeling that the bladder isn’t empty after urinating
- Leaking urine when sneezing or coughing
- Sensation of heaviness, aching or pain in the lower pelvis
- Feeling pressure or a physical bulge in the vaginal area
- Pain or discomfort with sexual intercourse – feels like there is a “block”
Please note that having one or more of these symptoms does not definitively mean that you have a cystocele. Many of the above can be associated with other conditions as well. If you are experiencing any of the above, we recommend seeing your physician to discuss what you are noticing and requesting a script for an evaluation by a Pelvic Floor Physical Therapist if appropriate. If you don’t have a physician, you can also schedule an appointment with one our therapist for an evaluation to determine if further treatment is necessary.
Stay tuned for our next chapter of Taking the Fear Factor out of…..when we discuss (rectocele, vulvodynia, vestibulodynia, etc)

What’s up, just wanted to say, I enjoyed this blog post.
It was inspiring. Keep on posting!
Thank you!
Perfectly written subject material, Really enjoyed looking through.
Glad you enjoyed it!